So I finally wrote up the story of Nora and Juney’s birth. It’s long but I make no apology for this – lots of things happened.
Content warning: This post talks about the death of a child.
A woman’s body may be designed for birth and pregnancy but we’re not built to carry twins. The last trimester of pregnancy was not kind to me. The babies just took and took until I felt like a half-person at best. I was absolutely enormous. I was exhausted all the time. I had to give up my job earlier than I wanted, at only six months pregnant, as I could no longer make the five minute walk between the bus stop and work without sitting down for a rest halfway. After that I was home alone most of the time and played a lot of video games.
I couldn’t do anything – by 30 weeks pregnant I couldn’t even make it all the way around the supermarket. I had the usual nesting urges but couldn’t bend to vacuum or dust. I spent half of every day lying in bed, too nauseous to get up, and the other half eating, insatiable. One of my most vivid memories of late pregnancy is listening to music in the shower and crying because I realised that the song was beautiful. (Nigel Kennedy – Solitude (For Yehudi Menuhin)). I know, I know, super melodramatic, but it was the first time in days that I’d felt any pleasure. So it wasn’t much of a life and I was relieved when the time was upon us. And I was booked in for a elective c-section, so once it was time, it was really time.
I was glad to be scheduled for a c-section. I mean, I wasn’t only glad. There aren’t many straightforward emotions about childbirth. I was scared of the surgery, dreading the pain. I was irritated that this choice was made for me, although I wouldn’t have chosen differently. But I was mostly glad. A year and a half before Nora and June were born, my infant niece died from brain trauma caused by lack of oxygen while my cousin was in labour with her. It is a long story, but she was the victim of a series of bad decisions and mistakes made by hospital staff. Losing Ellie was incredibly painful for the whole family. Her poor parents have suffered unimaginably. A well-timed c-section would have saved her life.
So, obviously, I was never going to romanticise vaginal birth. It seems to me that there are no “good” birthing options, any way you do it entails risk and pain, but at least an elective c-section pretty much guarantees that you get to take your baby home. I’m no longer able to see anything else as being important.
And anyway it’s not like I had a choice. The lead twin (the twin closest to the cervix) was transverse/breech for the entire pregnancy. She just got stuck that way. Nobody wanted to risk vaginal birth. My midwife went from “when they change position then we’ll talk about a birth plan” to, “so, I’ve booked your c-section with the hospital”. I feel lucky to live in a country where access to such a vital and life-saving surgery is a given (and free!).
And I liked that it was simple, straightforward. Like making a dinner reservation. I’m highly-strung and not great with uncertainty at the best of times. So there’s me in the past, all too aware of how things can go wrong during birth, nodding to herself. Yes. Good. It’s all sorted. I really liked that. “Book a flight down for the birth” I told my father-in-law. “Even if you can only manage a few days, it’ll be fine. It’s all booked in like theatre tickets”.
Oh, how fate must have laughed.

I got a steroid shot in the bottom at t-minus two days. The next day I went out for lunch with my cousin to celebrate my last day as a non-parent. I had a lemonade at lunch and the kids got all worked up from the sugar. This is deeply uncomfortable with two full-sized babies inside you. I was seriously ready to not be pregnant anymore.
After dinner that night I took a pill for the surgery then went nil-by-mouth. On Friday we woke at five, I fought through the morning sickness that still plagued me at 38 weeks pregnant to take a shower, and we got in the car and drove to Wellington hospital. We listened to our favourite songs and debated what would be the first song we played to our children once they were finally out in the world. (Barnaby – Bridge Over Troubled Water by Simon and Garfunkle vs Me – To the Great Unknown by Cloud Cult). I was so excited I was close to tears the whole trip.
We got to the hospital and we waited. Our midwife Julie arrived, my parents arrived. We’d asked them to be there to support us. Someone took us all through to a delivery room and we waited a whole lot more. We did a crossword and everyone but me had tea and biscuits. Time wore on and by mid-morning it was clear there was a problem. To make a long story shorter, I did not have the children that day. There was absolutely no room in the hospital for us, not in the operating theatre or in the delivery ward, not in the maternity ward. They’d had an unusually large number of emergencies come in and they had to take priority.

The consulting obstetrician sat us down to discuss other options. They were having trouble re-booking us. It was November third, a Friday. Wellington hospital doesn’t do elective c-sections on the weekend. Monday and Tuesday were already booked solid. Leaving it until Wednesday was too risky: 38 weeks is considered “full term” for twins because after that point the incidence of placental failure increases daily. But despite all this, the obstetrician was pleased. He’d found a way to have the c-section that day. The other hospital in our area had room for us and the consultant there was willing. We just had to agree and they’d transfer us.
The other hospital was the hospital where the mistakes were made that caused the death of my little niece. I still kept an open mind. We were kind of desperate, after all. “Remember, what happened to your cousin was very different circumstances” said Julie. True. I prepared myself to be even further from home and to be without our excellent midwife, who was not licensed to work in that hospital. But then we found out the name of the consultant who was to perform my operation. It was the consultant who was on call the night my niece was born. The person who made the worst of the bad decisions. The person who bears the brunt of the blame.
The very same doctor.
As worried as I was for our children, as aware as I was that they were at risk, I couldn’t possibly go through with that. I didn’t even trust myself to be in the same room as that person. The consultant in Wellington was very kind through the million tears it took me to explain all this. He respected that this was a case of trauma (interestingly, I’d never thought of it that way until he said that word) and he made a note in my file to ensure that medical staff on other shifts wouldn’t raise this as an option with me again.
It was an awful discussion, but it’s funny how the brain works in these peak moments. I remember very clearly having a wee moment of levity, sitting in my hospital bed and looking at all the faces that surrounded me as we talked it through, the doctors and midwives grave, my husband serious, my father pale, my mother weeping. Oh my god! I thought. I’m living in a medieval tableau!
But what to do? “You might just have to go into labour”, joked Julie. “Then they’ll have to make room for you”. She’d previously told me that if I went into labour it was a medical emergency of the call-an-ambulance kind, so this wasn’t exactly reassuring. (Given the position of the babies and how fast twin labour can progress, there was a chance that Nora’s umbilical cord would fall out my cervix and then be squashed by her bottom as she tried to follow it, cutting off her oxygen)
Anyway, the only thing left to do was try and get it done the next day. Through no fault of my own, I’d become a Special Case and Exceptions would have to be made. In other words, I was a problem. At least, that was the attitude of the hospital midwife the next morning when we returned for our elective c-section – on a Saturday, of all days!
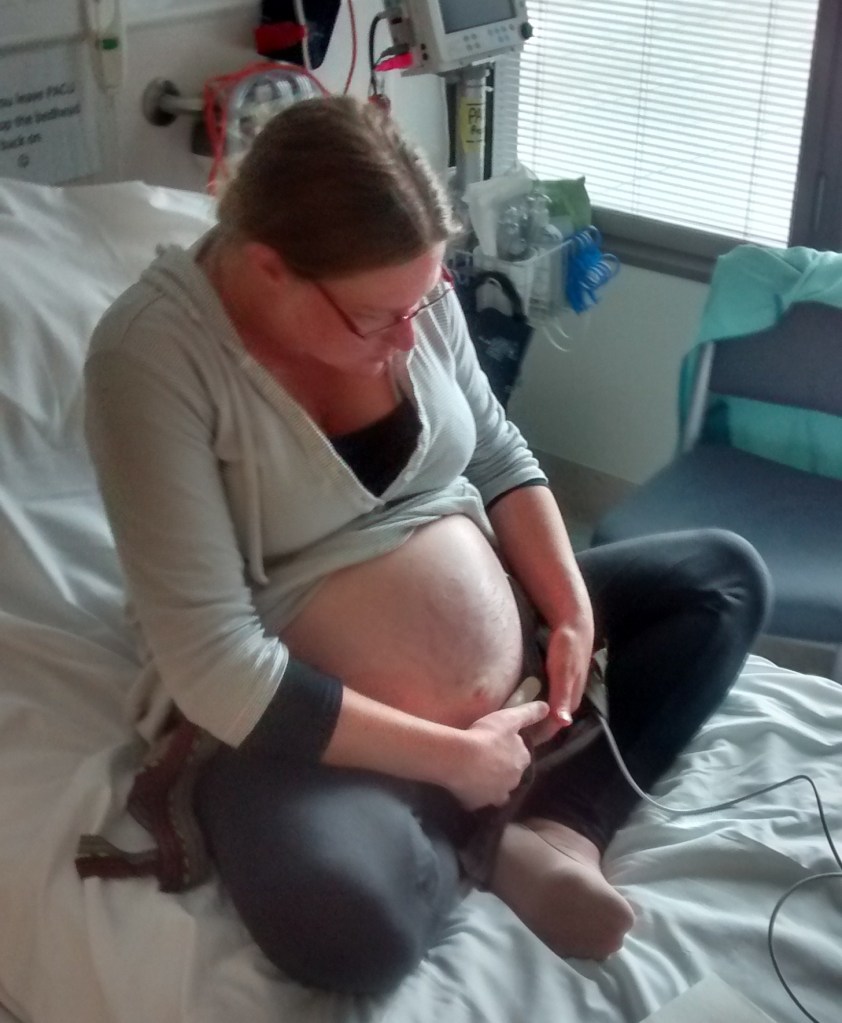
We once again waited around for half a day. I was shaved for surgery and put in a hospital gown. But the hospital was still at capacity and we never even spoke to that day’s obstetrician before they sent us away again. Starving, we went out for lunch with my parents, my mother-in-law, and my poor father-in-law, who had to get on a flight back to Auckland immediately afterwards, his grandchildren still unmet. The heavy atmosphere of that awful meal is burned irrevocably into my brain. I mean, I went out for one last brunch with my ex-boyfriend the day before I was to board a plane back to New Zealand from Taiwan and leave him forever, and that meal was waaaaay less heavy with unspoken sorrow and tension.

After we left the cafe a woman called me a “fat cow” because I held up her car for milliseconds while I waddled across the road. The world seemed a cold and uncaring place that day. Also, and this still annoys me because I’m pedantic, I was not fat but like the most pregnant a person could possibly be. I was visibly the world’s most pregnant person. Was she an idiot?
As we parted I forbade my parents from coming to the hospital the next day unless the children had actually been born. They had gone all grey and limp like old dish rags after two full days of waiting in the family room, worrying, ready to spring into action at a moment’s notice. Mum was… not thrilled. Poor mum. She so desperately wanted to be of use to us.
With another day ticking past the risk to our children was growing. Trying to keep our spirits up, Barns and I decided that we’d go see Thor: Ragnarok the next day after the hospital sent us away again, and then for the third day running I went nil-by-mouth after dinner. I slept poorly that night, kept awake by the wheezing sound of my own breathing, kids by that point so enormous my lungs were constricted when I lay down. I wound up sleeping semi-upright in a chair. Barns left the bed to be near me on our sofa. That was a nice thing about pregnancy. No matter how hard it got or how much more he had to take on (cutting my toenails was just the start of it), Barnaby supported me every step of the way and never complained.
At least we were allowed an hour’s extra sleep that morning. “Never mind the usual reporting time, just come in at 8am”, we were told. “We know you’re coming”. Oh, so comforting. We couldn’t manage music on the drive that time.

The atmosphere in Wellington Hospital was rather different on Sunday. “This is ridiculous!” raged that day’s consulting obstetrician (the third, if you’re keeping count). “I can’t believe they’re doing this to you! Well, I’m going to make them sort it out. I’ll get the head of NICU to come and explain things to you. You just wait here”.
While we were grateful that someone had taken up our cause, he left without explaining what the NICU (neonatal intensive care unit) had to do with anything and we were bewildered – as far as we knew, our babies were full-term and perfectly healthy. But the head of NICU, who, astonishingly, did come in for us, explained that twins are statistically more likely to need help after birth and despite the risk to the placenta, the babies were safer inside than out unless the NICU had two free incubators. There was finally room in the operating theatre, Delivery and Maternity, but the NICU was chokka.
“I’m going to see what I can do. They have room in the SCBU (Special Care Baby Unit) at Hutt Hospital so if I can transfer some of our patients out there then there’ll be room for your babies here. But this is over my level so I’ve got to get the head of Wellington Hospital to call the head of Hutt Hospital. It all takes a bit longer because it’s Sunday but I’ll know by 2pm at the latest”.
Goodness! All this bother for us! I felt a little guilty – I’ve heard that the SCBU is a lot less comfortable for parents than the NICU. If the parents who had to move because of us ever read this, I’m sorry!
I was still nil-by-mouth so they hooked me up to a drip to stave off dehydration and left us alone for hours. The only things I remember doing in that time is taking photos of my feet, one of which had puffed up like a balloon.

And getting into a hospital gown, yet again.

At around 2:15pm, a midwife burst into the room.
“Let’s move. We’ve got a spot for you but we’ve got to do it right now”.
And just like that, we were off. I couldn’t believe I had to go start my life as a parent in the state I was in. For one I was shell-shocked from the stress. Worse, as I hadn’t been allowed to eat or drink anything for the majority of the last three days whilst heavily pregnant and travelling back and forth to the hospital, I was already utterly exhausted. I wasn’t capable of feeling excited about meeting the babies or nervous about the surgery or relieved things were finally sorted out. I did however manage a brief pang of regret that I wouldn’t get to go see Thor: Ragnarok, so make of that what you will.
The operating theatre was startlingly unlike the ones you see on telly – I literally walked to the operating table and it had a curtain instead of a door. The anaesthesiologists did their thing and soon I was shaking uncontrollably (which is apparently normal) while the surgeon sliced me open. I couldn’t cope with looking in the direction of my stomach at that point so I watched Barnaby’s face as our children were carefully lifted into the world. I wish I could write more profoundly about this stuff but I am only able to say that he looked really happy.
June flipped over as soon as her sister was out of the way (poor kids had been squashed for months) and so they both came into the world bum-first. They were checked and pronounced perfectly healthy. After all that trouble, the beds in NICU were not needed, and thank goodness for that. They were weighed and then weighed again because they were the exact same weight and that confused everyone. They were placed on my chest while I was stitched up. I could see one face with the lovely dark eyes of all newborns but I could only see the top of the other child’s head.
“I can’t see her face,” I told Barnaby. He patted my hand.
“The baby. I can’t see her face”, I told Julie. She gave me a sympathetic look. I understood this to mean that seeing my child for the first time was lesser in importance to not disturbing the surgeon while he was trying to sew my guts back together but I was still a bit sad about it.

Eventually the kids went off with their father and I was wheeled into recovery where five or six people gathered around the bed to stare at (brace yourselves) my vagina. Honestly I wasn’t thrilled about this but they all seemed really worried about me so I decided not to mention it.
“She’s trickling”, one of them said. Trickling was obviously bad. The solution to trickling turned out to be massaging my stomach to get my womb to contract, and when this didn’t work, pounding me on the abdomen so firmly that it was disturbing not to be able to feel it. Once that was sorted the gaggle of doctors was replaced with a bundle of midwives and my vagina swapped with my boobs, at least in terms of being out for the whole world to see. I needed quite a lot of help (literally five people) but soon I was breastfeeding! Actually breastfeeding! Me! Astonishing. The midwives left me to it and I finally had a peaceful moment with my little ones. I could even see their dear faces. They were skinny wee things with only a bit of fluff on their heads. Long fingers. They were so sleepy.
I wish I could leave it there, a small and cosy scene, but sadly I have more difficult events to process through this free form of therapy.
As we were snuggling I became worried that I was going to drop the kids. It seemed difficult to get my arms to do what I wanted them to do. This…didn’t seem… to be a normal worry… so I thought about it for a while…but my thoughts were moving… very slowly. Oh dear… I think…this is bad…and shouldn’t be happening… I should… tell someone.
“Excuse me. Can somebody come take the babies? I don’t feel right”.
The nurse’s face when she glanced at my vital signs was enough to tell me I’d been correct to call out. The babies were rushed away.
The next five hours are a bit blurry so I’m not sure what order any of this happened in, but anyway: My heart rate was well below normal. The medication to fix this put me into atrial fibrillation. My blood pressure fluctuated wildly. My blood oxygen saturation dropped. None of the medical staff seemed overly worried but I was mildly concerned that I was about to die. I would have appreciated it if my husband was holding my hand but he was nowhere to be seen. I later found out that the midwives were keeping him busy – and out of the way – by teaching him how to put on nappies and dress the babies.

At some point the morphine wore off and I was in terrible pain. Apparently it was worse than the usual post-cesarean pain because of the surgeon slamming my stomach when he was trying to get my womb to contract. I wasn’t allowed more morphine. They give you two doses of morphine, an instant one and a slow-release one, and the slow-release one was in my body, it just hadn’t kicked in yet. So they gave me…paracetamol. As you may guess, it didn’t do shit. Also my blood sugar tanked, which was actually brilliant: they gave me two lemonade popsicles, the first things I’d consumed in 24 hours. I can’t imagine enjoying anything more than I enjoyed those popsicles. This is when Barns reappeared – while I was scoffing ice blocks – so it took a while for him to fully comprehend that scary things were happening.
This all sounds very urgent but actually it happened over several hours while I mostly just lay around and felt dreadful. The kids considerately napped in the corner. At some point the head of NICU dropped by to congratulate us (I swear, the doctors, nurses and midwives in this story do all have names but I can’t remember a single one of them). I remember apologising to her because Nora and June didn’t need to go to the NICU after all her efforts, and she just laughed. She pointed out that doctors do actually hope for good outcomes for patients, but said it kindly and didn’t make me feel like an idiot at all.
We had texted my parents and my mother-in-law when I went into the surgery and they diligently jumped in their cars and sped to the hospital so they were sitting in the family room waiting all the time I was not dying. The hospital staff felt so sorry for them that they convinced Barnaby, over my objections, to take the kids out to meet them. I like to imagine that they were happy to meet their grand kids but I get the feeling my parents were so worried about me that they were rather distracted.

Eventually everything was sorted out but the blood oxygen. Barns and I were actually talking about this recently and we had both been thinking, oxygen saturation is at 91%, right? That is quite a lot, what’s the big deal? And then Barns read an article about Covid19 which mentioned how Covid patients would show up at the hospital with similar stats and the doctors would freak out, so I suppose it was pretty low after all.
The anaesthesiologist explained that she must have given me a bit too much juice in my epidural and so my lungs were probably a bit crumpled or something. I don’t know. We had to wait for an x-ray but it could probably all be fixed by my taking a few big breaths. That was all they were asking and I was incapable of it. The second round of morphine still hadn’t kicked in and I couldn’t bear the pain of deep breathing. If she’d upped my painkillers I might have tried but she wouldn’t and so we were at a stalemate. Still, she must have been feeling guilty about it because she decided to let my parents come into Recovery to see me. This seems to be a big hospital no-no. The head midwife was deeply opposed and the anaesthesiologist just straight-out stated that she was a higher rank and so it was happening. Barns and I pretended very hard not to watch the ensuing argument.
I don’t know how bad I looked but my parents looked like the walking dead. They’ve never coped well with worry for me. I sent them home again.
Finally, after 5 hours, they decided 98% saturation was good enough and it would fix itself overnight once my morphine kicked in (it did!). I was released to the delivery ward on oxygen. It was past 8pm. I ate something – a sandwich? yogurt? – and a trundle bed was set up for Barnaby, and then sleep took me and wouldn’t let me go until the next morning. I’m pretty sure that one of the reasons they usually do elective c-sections at 8 in the morning is to avoid this exact scenario. I was in no fit state to tend to the babies. Somebody – Barns tells me it was him and a couple of midwives – looked after the kids overnight and I’ll forever be grateful for that because I just couldn’t. I had nothing left.
So, the birth of my kids isn’t a super happy story. I know things could have been much worse, please believe me that I know this. I am aware that we have a lot to be grateful for. But honestly it was the most stressful thing I’ve ever experienced by a large margin. I in no way blame the hospital staff for how things played out. One common thread of the experience was that everyone was doing their absolute best for us. They were in a difficult situation, too, although they tried a lot harder to hide it.
It also wasn’t much of a bonding experience. In fact, you have probably noticed that the children are barely in this story. I remember though having the sense that I loved them greatly when they were very small, in fact being sure of it, because nobody could put up with all the newborn tribulations if they didn’t truly love their kids. And now we’re healthily close so it all seems like so much water under the bridge these days.

We spent five days in the hospital which was such a shit show that it would need a whole other blog post, except I was exhausted and on morphine for most of it so I don’t think I could put it in chronological order. I do have a few things I want to say about it, though:
- Please, somebody, please give our health system more money. These poor doctors and nurses and midwives are working so hard with so little. I know we were in the hospital at an unusually busy time but there has to, has to, be a better way of doing things than putting babies’ lives at risk by postponing a c-section because there’s literally no space in hospital. And surely we can do better than having scared new parents wait forty minutes at 3 in the morning for a nurse to be available to bring some formula for a crying newborn. Or not having enough staff to keep track of when patients need painkillers, which resulted in me having to go back on morphine 3 days after my surgery and Barns, who frankly already had quite a lot on his plate, having to monitor all my medication for the rest of my stay. Surely, New Zealand, we can do better than that.
- I told my dad that the shadows on the tap were moving and I wasn’t sure if it was morphine or ghosts and he was obviously the wrong person to ask because he told me in earnest that it was probably both. “Lots of ghosts in a hospital”.
- If you have a c-section then remember I told you to start on the Kiwi Crush early. Don’t wait until you have a problem.
- Not surprisingly, it took a while for me to piece myself back together after the surgery. Barnaby rose to the occasion magnificently. Once we got home from the hospital he had to teach me how to change nappies and make formula because he’d done it all up until that point. He is a truly wonderful dad and I was awfully proud of him.

- I got my first lesson in trusting myself as a parent watching a midwife try to work out why my baby was still crying after she’d just had a feed.
“Maybe she’s still hungry?” I ventured.
“She shouldn’t be still hungry! Her stomach is the size of a pea. Her nappy is fine…maybe she wants her glove back on, it fell off. Or do you want a blanket, bubba?”
I didn’t like to argue with the professional but I wasn’t convinced. I mean, I’m her mother and I’m always hungry. I was quickly proven right, and this was a useful thing to learn early on.
- On around day two or three of my children’s lives, I was lying in bed in the quiet of the morning and I felt eyes on me. I looked up to see Nora watching me through the Plexiglas of her bassinet. She just lay there calmly and I locked eyes with her, caught up in, I like to imagine, similar wonder. Oh wow, I thought. I’m her mum!

